Mumps seroprevalence and molecular epidemiology
Project leader: Judith Huebschen, Antony Black, Claude Muller
Member of staff: Keooudomphone Vilivong, Chanthasone Souvannaso
Background
Mumps is a vaccine preventable disease caused by mumps virus (family: Paramyxoviridae, genus: Rubulavirus) with a subclinical course in up to one third of all cases. Common manifestations include parotitis and respiratory symptoms; and orchitis in postpubertal males. Laboratory diagnosis relies on detection of specific IgM antibodies or mumps virus RNA. Based on 316 nucleotides covering the small hydrophobic (SH) gene region, 12 different genotypes of mumps virus have been proposed with genotypes C, F, G and H predominating in Asia. In 2012, 120 out of 194 WHO member states (62%) were using mumps vaccine in their national immunization schedule. In Lao PDR, mumps is not a notifiable disease and mumps vaccine is currently not included in the routine childhood immunization program.
Activities and Prospective
In order to assess the burden of disease, we investigated the seroprevalence of mumps-specific IgG antibodies across four provinces. In addition, we continue to genetically characterize mumps viruses from outbreaks and single cases brought to our attention by the National Center for Laboratory and Epidemiology (NCLE) and medical doctors. Blood and/or throat swabs from suspected cases are investigated for specific IgM antibodies or viral RNA.
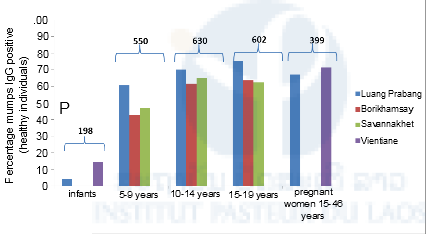
Mumps cases to date have occurred between March and November in 2011-2013 and 5-15 year olds were most affected. Four sequences from an outbreak in the North of Lao PDR in 2011 were identical and belonged to genotype G. Eight sequences from two outbreaks and wo individual cases from 2012 and 2013 belonged to genotype J. In addition, sera collected from 2379 healthy infants and school pupils between 9 months and 19 years and from pregnant women between 16 and 46 years were investigated for mumps-specific IgG. Overall, 58.2% were positive, 39.5% were negative and the remaining 2.3% were equivocal. The seropositivity increased with age, with the lowest percentage found in the <1 year old infants (9.1%) and the highest in the cohort of pregnant women (69.2%). More females than males were seropositive (60.4 versus 54.9%). There were some differences between the locations.
Swab and serum samples from suspected cases continue to be collected and analyzed in ongoing active mumps surveillance in collaboration with NCLE.
These data will be presented as a poster at the 12th International Conference on Molecular Epidemiology and Evolutionary Genetics of Infectious Diseases, Bangkok, 11-13 December, 2014
Partners
+ Department of Pathology, University of Health Sciences, Vientiane, Lao PDR.
+ Luangprabang Provincial Hospital, Luangprabang, Lao PDR.
+ Department of Pathology, Faculty of Medicine, Chiang Mai University, Thailand.
+ WHO Lao Country Office, Vientiane, Lao PDR.
+ National Center for Laboratory and Epidemiology, Vientiane, Lao PDR.
+ Public Health Laboratory Services Branch, Centre for Health Protection, Department of Health, Hong Kong SAR, China.
Publication
Hubschen JM, Vilivong K, Souvannaso C, Black AP, Lutteke N, Samountry B, Phongsavath V, Khamphaphongphane B, Denny J, Sayyavong C, et al: High prevalence of mumps in Lao People’s Democratic Republic. Clinical microbiology and infection, February 2014.
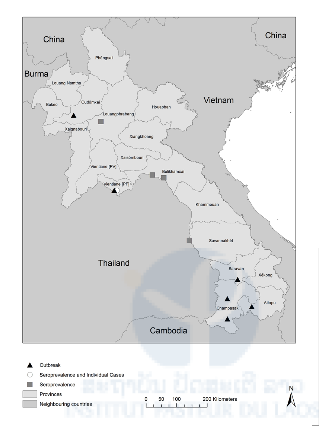
Figure 1: Map of Lao PDR showing the different sample collection sites for mumps seroprevalence and case molecular characterisation. PV = province; PF = prefecture.

Figure 2: Phylogenetic tree based on 316 nucleotides of the mumps virus SH gene region and the Kimura 2-parameter model and the Neighbor-Joining algorithm. Light grey dots mark the sequences obtained from the mumps outbreak in 2011, grey triangles highlight sequences from the 2012 outbreak and black diamonds show sequences from the 2013 outbreak. The grey square and the black triangle mark the individual cases from 2012 and 2013, respectively. White dots indicate the closest relatives of the sequences from Lao PDR identified by BLAST.